lower-back-pain
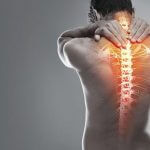
The spine is made of 33 individual bones stacked one on top of the other. Ligaments and muscles connect the bones together and keep them aligned.The spinal column provides the main support for your body, allowing you to stand upright, bend, and twist. Protected deep inside the bones, the spinal cord connects your body to the brain, allowing movement of your arms and legs. Strong muscles and bones, flexible tendons and ligaments, and sensitive nerves contribute to a healthy spine. Keeping your spine healthy is vital if you want to live an active life without back pain.
Spinal curves
When viewed from the side, an adult spine has a natural S-shaped curve. The neck (cervical) and low back (lumbar) regions have a slight concave curve, and the thoracic and sacral regions have a gentle convex curve . The curves work like a coiled spring to absorb shock, maintain balance, and allow range of motion throughout the spinal column.
The muscles and correct posture maintain the natural spinal curves. Good posture involves training your body to stand, walk, sit, and lie so that the least amount of strain is placed on the spine during movement or weight-bearing activities . Excess body weight, weak muscles, and other forces can pull at the spine’s alignment:
- An abnormal curve of the lumbar spine is lordosis, also called sway back.
- An abnormal curve of the thoracic spine is kyphosis, also called hunchback.
- An abnormal curve from side-to-side is called scoliosis.
Muscles
The two main muscle groups that affect the spine are extensors and flexors. The extensor muscles enable us to stand up and lift objects. The extensors are attached to the back of the spine. The flexor muscles are in the front and include the abdominal muscles. These muscles enable us to flex, or bend forward, and are important in lifting and controlling the arch in the lower back.
The back muscles stabilize your spine. Something as common as poor muscle tone or a large belly can pull your entire body out of alignment. Misalignment puts incredible strain on the spine
Vertebrae
Vertebrae are the 33 individual bones that interlock with each other to form the spinal column. The vertebrae are numbered and divided into regions: cervical, thoracic, lumbar, sacrum, and coccyx . Only the top 24 bones are moveable; the vertebrae of the sacrum and coccyx are fused. The vertebrae in each region have unique features that help them perform their main functions.
Cervical (neck) – the main function of the cervical spine is to support the weight of the head (about 10 pounds). The seven cervical vertebrae are numbered C1 to C7. The neck has the greatest range of motion because of two specialized vertebrae that connect to the skull. The first vertebra (C1) is the ring-shaped atlas that connects directly to the skull. This joint allows for the nodding or “yes” motion of the head. The second vertebra (C2) is the peg-shaped axis, which has a projection called the odontoid, that the atlas pivots around. This joint allows for the side-to-side or “no” motion of the head.
Thoracic (mid back) – the main function of the thoracic spine is to hold the rib cage and protect the heart and lungs. The twelve thoracic vertebrae are numbered T1 to T12. The range of motion in the thoracic spine is limited.
Lumbar (low back) – the main function of the lumbar spine is to bear the weight of the body. The five lumbar vertebrae are numbered L1 to L5. These vertebrae are much larger in size to absorb the stress of lifting and carrying heavy objects.
Sacrum – the main function of the sacrum is to connect the spine to the hip bones (iliac). There are five sacral vertebrae, which are fused together. Together with the iliac bones, they form a ring called the pelvic girdle.
Coccyx region – the four fused bones of the coccyx or tailbone provide attachment for ligaments and muscles of the pelvic floor.
- a drum-shaped body designed to bear weight and withstand compression (purple)
- an arch-shaped bone that protects the spinal cord (green)
- star-shaped processes designed as outriggers for muscle attachment (tan)
Intervertebral discs
Each vertebra in your spine is separated and cushioned by an intervertebral disc, keeping the bones from rubbing together. Discs are designed like a radial car tire. The outer ring, called the annulus, has criss-crossing fibrous bands, much like a tire tread. These bands attach between the bodies of each vertebra. Inside the disc is a gel-filled center called the nucleus, .
Discs function like coiled springs. The criss-crossing fibers of the annulus pull the vertebral bodies together against the elastic resistance of the gel-filled nucleus. The nucleus acts like a ball-bearing when you move, allowing the vertebral bodies to roll over the incompressible gel. The gel-filled nucleus is composed mostly of fluid. This fluid absorbed during the night as you lie down and is pushed out during the day as you move upright.
With age, our discs increasingly lose the ability to reabsorb fluid and become brittle and flatter; this is why we get shorter as we grow older. Also diseases, such as osteoarthritis and osteoporosis, cause bone spurs (osteophytes) to grow. Injury and strain can cause discs to bulge or herniate, a condition in which the nucleus is pushed out through the annulus to compress the nerve roots causing back pain.
Vertebral arch & spinal canal
On the back of each vertebra are bony projections that form the vertebral arch. The arch is made of two supporting pedicles and two laminae . The hollow spinal canal contains the spinal cord, fat, ligaments, and blood vessels. Under each pedicle, a pair of spinal nerves exits the spinal cord and pass through the intervertebral foramen to branch out to your body.
Surgeons often remove the lamina of the vertebral arch (laminectomy) to access and decompress the spinal cord and nerves to treat spinal stenosis, tumors, or herniated discs.
Seven processes arise from the vertebral arch: the spinous process, two transverse processes, two superior facets, and two inferior facets.
Facet joints
The facet joints of the spine allow back motion. Each vertebra has four facet joints, one pair that connects to the vertebra above (superior facets) and one pair that connects to the vertebra below
Ligaments
The ligaments are strong fibrous bands that hold the vertebrae together, stabilize the spine, and protect the discs. The three major ligaments of the spine are the ligamentum flavum, anterior longitudinal ligament (ALL), and posterior longitudinal ligament (PLL) . The ALL and PLL are continuous bands that run from the top to the bottom of the spinal column along the vertebral bodies. They prevent excessive movement of the vertebral bones. The ligamentum flavum attaches between the lamina of each vertebra.
Spinal cord
The spinal cord is about 18 inches long and is the thickness of your thumb. It runs within the protective spinal canal from the brainstem to the 1st lumbar vertebra. At the end of the spinal cord, the cord fibers separate into the cauda equina and continue down through the spinal canal to your tailbone before branching off to your legs and feet. The spinal cord serves as an information super-highway, relaying messages between the brain and the body. The brain sends motor messages to the limbs and body through the spinal cord allowing for movement. The limbs and body send sensory messages to the brain through the spinal cord about what we feel and touch. Sometimes the spinal cord can react without sending information to the brain. These special pathways, called spinal reflexes, are designed to immediately protect our body from harm.
The nerve cells that make up your spinal cord itself are called upper motor neurons. The nerves that branch off your spinal cord down your back and neck are called lower motor neurons. These nerves exit between each of your vertebrae and go to all parts of your body.
Any damage to the spinal cord can result in a loss of sensory and motor function below the level of injury. For example, an injury to the thoracic or lumbar area may cause motor and sensory loss of the legs and trunk (called paraplegia). An injury to the cervical (neck) area may cause sensory and motor loss of the arms and legs (called tetraplegia, formerly known as quadriplegia).
Spinal nerves
Thirty-one pairs of spinal nerves branch off the spinal cord. The spinal nerves act as “telephone lines,” carrying messages back and forth between your body and spinal cord to control sensation and movement. Each spinal nerve has two roots (Fig. 8). The ventral (front) root carries motor impulses from the brain and the dorsal (back) root carries sensory impulses to the brain. The ventral and dorsal roots fuse together to form a spinal nerve, which travels down the spinal canal, alongside the cord, until it reaches its exit hole – the intervertebral foramen . Once the nerve passes through the intervertebral foramen, it branches; each branch has both motor and sensory fibers. The smaller branch (called the posterior primary ramus) turns posteriorly to supply the skin and muscles of the back of the body. The larger branch (called the anterior primary ramus) turns anteriorly to supply the skin and muscles of the front of the body and forms most of the major nerves.
The spinal nerves are numbered according to the vertebrae above which it exits the spinal canal. The 8 cervical spinal nerves are C1 through C8, the 12 thoracic spinal nerves are T1 through T12, the 5 lumbar spinal nerves are L1 through L5, and the 5 sacral spinal nerves are S1 through S5. There is 1 coccygeal nerve.
The spinal nerves innervate specific areas and form a striped pattern across the body called dermatomes (Fig. 10). Doctors use this pattern to diagnose the location of a spinal problem based on the area of pain or muscle weakness. For example leg pain (sciatica) usually indicates a problem near the L4-S3 nerves.
Herniated disk in the lower back
What is lumbar disk disease (herniated disk, ruptured disk or bulging disk)?
As we age, the intervertebral disk may lose fluid and become dried out. As this happens, the disk compresses. This may lead to the deterioration of the tough outer ring allowing the nucleus, or the inside of the ring, to bulge out. This is considered a bulging disk.
As the disk continues to degenerate, or with continued stress on the spine, the inner nucleus pulposus may actually rupture out from the annulus. This is considered a ruptured, or herniated, disk. The fragments of disk material can then press on the nerve roots that are located just behind the disk space. This can cause pain, weakness, numbness, or changes in sensation.
Most disk herniations happen at the lower lumbar spine, especially at the L4-5 and L5-S1 levels.
What causes lumbar disk disease?
Lumbar disk disease is due to a change in the structure of the normal disk. Most of the time, disk disease comes as a result of aging and the degeneration that occurs within the disk. Occasionally, severe trauma can cause a normal disk to herniate. Trauma may also cause an already herniated disk to worsen.
What are the symptoms of lumbar disk disease?
The symptoms of lumbar disk disease vary depending on where the disk has herniated, and what nerve root it is pushing on. The following are the most common symptoms of lumbar disk disease. However, each individual may experience different symptoms. Symptoms may include:
- Intermittent or continuous back pain. This may be made worse by movement, coughing, sneezing, or standing for long periods of time.
- Spasm of the back muscles
- Sciatica. Pain that starts near the back or buttock and travels down the leg to the calf or into the foot.
- Muscle weakness in the legs
- Numbness in the leg or foot
- Decreased reflexes at the knee or ankle
- Changes in bladder or bowel function
The symptoms of lumbar disk disease may resemble other conditions or medical problems. Always consult your health care provider for a diagnos
Fractures of the thoracic and lumbar spaine
Vertebral Compression Fracture
A vertebral compression fracture refers to a break of the vertebral body, most often below the T7 level of the thoracic spine (upper back), and is most commonly caused by weakened bone resulting from osteoporosis. Most vertebral compression fractures result in a loss of more than 15% to 20% of the height of the vertebra.
See What You Need to Know About Osteoporosis
Fractures in weakened vertebrae can occur in the course of normal physical activities, without significant accident or injury. At the time of fracture, there is often a sudden onset of back pain. When the fracture heals, there is often a residual wedge-shape of the typically square vertebrae (spine bone). Suffering one vertebral compression fracture increases the risk of future vertebral compression fractures, which can cause unwanted side effects such as significant height loss, spinal deformity (kyphosis, or hunchback), and even has the potential to shorten one’s lifespan if left untreated.
Back Pain in Children
Back pain in children is not like back pain in adults. Compared to an adult, a child with a backache is more likely to have a serious underlying disorder. This is especially true if the child is 4 years old or younger, or if a child of any age has back pain accompanied by:
- Fever or weight loss
- Weakness or numbness
- Trouble walking
- Pain that radiates down one or both legs
- Bowel or bladder problems
- Pain that keeps the child from sleeping
More serious causes of back pain need early identification and treatment or they may become worse. Always see a doctor if your young child’s back pain lasts for more than several days or progressively worsens
Kyphosis (Roundback) of the Spine
Some degree of rounded curvature of the spine is normal. The term kyphosis is used to describe the spinal curve that results in an abnormally rounded back.
Diagnosis
A visit to the doctor is typically brought on by a scoliosis screening examination at school, a child’s or parent’s concern about the cosmetic deformity of a rounded back, or pain
The doctor may ask the child to bend forward so that the slope of the spine can be assessed. X-rays of the spine will show if there are any bony abnormalities. X-rays will also help measure the degree of the kyphotic curve. A kyphotic curve that is more than 50° is considered abnormal
Types of Kyphosis
Postural Kyphosis
Postural kyphosis is the most common type of kyphosis. It is often attributed to slouching. It represents an exaggerated, but flexible, increase of the natural curve of the spine
Postural kyphosis usually becomes noticeable during adolescence. It is more common among girls than boys. It rarely causes pain
Although exercise to strengthen the abdomen and stretch the hamstrings may help relieve associated discomfort, it is unlikely to result in significant correction of the postural kyphosis. With occasional exceptions, postural kyphosis does not lead to problems in adult life
Scheuermann’s Kyphosis
Scheuermann’s kyphosis is named after the Danish radiologist who first described the condition
As with postural kyphosis, Scheuermann’s kyphosis often becomes apparent during the teen years; however, patients with Scheuermann’s kyphosis have a significantly more severe deformity, particularly thin individuals.
Scheuermann’s kyphosis usually affects the upper (thoracic) spine. It can also occur in the lower (lumbar) back area. If pain is present, it is usually felt at the apex of the curve.
Activity can aggravate the pain, as can long periods of standing or sitting. Exercise and anti-inflammatory medication can help ease associated discomfort.
When x-rays of patients with kyphosis are examined, the vertebrae and disks will appear normal in those with postural kyphosis, but they will appear irregular and wedge-shaped in those with Scheuermann’s kyphosis.
Lower back pain is a common cause for visits to the doctor. According to the National Institute of Neurological Disorders and Stroke (NINDS), low back pain is the second most common neurological problem
Most low back pain is the result of an injury, such as muscle sprains or strains due to sudden movements or poor body mechanics while lifting heavy objects. But low back pain can also be caused by certain diseases, such as cancer of the spinal cord, ruptured or herniated disc, sciatica, arthritis, kidney infections, or infections of the spine. Acute back pain can last anywhere from a few days to a few weeks, while chronic back pain is pain that lasts longer than three months.
Lower back pain is more likely to occur in individuals between the ages of 30 and 50. This is partly due to the changes that occur in the body with aging. As you grow older, the fluid content between the vertebrae in the spine becomes reduced, which means discs in the spine are more easily irritated. Some muscle tone is also lost, which makes the back more prone to injury. This is why strengthening your back muscles and using good body mechanics are helpful in preventing lower back pain.
Causes of Lower Back Pain
Strains
The muscles and ligaments in the back can be stretched or torn due to over-activity. Symptoms include pain and stiffness in the lower back, as well as muscle spasms. These symptoms tend to be relieved with rest and physical therapy.
Disc Injury
The discs in the back are prone to injury, and this risk increases with age. The outside of the disc can be torn or may be herniated. A herniated disc (also called a slipped or ruptured disc) and occurs when the cartilage surrounding the disc pushes against the spinal cord or nerve roots. The cushion that sits between the spinal vertebrae is pushed outside its normal position. This can result in compression of the nerve root as it exits from the spinal cord and through the vertebral bones. Disc injury usually occurs suddenly after lifting something or twisting the back. Unlike a back strain, pain from a disc injury usually lasts for more than 72 hours.
Sciatica
Sciatica can occur with a herniated disc if the disc presses on the sciatic nerve. The sciatic nerve connects the spine to the legs. As a result, sciatica can cause pain in the legs and feet. This pain is usually felt as a burning or pins-and-needles sensation.
Spinal Stenosis
Spinal stenosis is when the spinal column narrows, putting pressure on the spinal cord and spinal nerves. Spinal stenosis is most commonly caused by degeneration of the discs between the vertebrae. The result is compression of the nerve roots or spinal cord by bony spurs or soft tissues, such as discs. Symptoms are usually caused by the pressure on the spinal nerves and may include numbness, cramping, and weakness. These symptoms may be felt anywhere in the body. Many people with spinal stenosis notice their symptoms worsen when standing or walking.
Abnormal Spine Curvatures
Scoliosis, kyphosis, and lordosis are all conditions that cause abnormal curvatures in the spine. These are congenital conditions and are usually diagnosed in children and teenagers. The abnormal curvature places pressure on the muscles, tendons, ligaments, and vertebrae, causing pain and poor posture.
Other Conditions
Along with the above conditions, there are a number of other conditions that cause lower back pain. These conditions include:
arthritis (Lumbar osteoarthritis is a very painful condition which affects the lower back)
fibromyalgia – long-term pain and tenderness in the joints, muscles, and tendons
spondylitis – inflammation of the joints between the spinal bones
spondylosis (spinal osteoarthritis) is a degenerative disorder that may cause loss of normal spinal structure and function. Although aging is the primary cause, the location and rate of degeneration is individual.
kidney and bladder problems (severe infections of the bladder can cause low back pain)
pregnancy (due to the increased strain on the lower back and the change in body posture)
endometriosis – a painful condition where cells from the uterus grow in other parts of the body
ovarian cysts – a fluid-filled growth on the inside or outside of an ovary
uterine fibroids – non-cancerous tumors in the uterus
cancer
Low Back Pain Tests
Most doctors begin by conducting a physical examination to determine where you are feeling the pain, as well as if your range of motion has been affected. Your doctor may also check your reflexes and your response to certain sensations. This is done to determine if your nerves are affected by your lower back problem. Unless you have concerning or debilitating symptoms, your doctor will probably monitor your condition for a few weeks before sending you for testing. This is because most lower back pain resolves using simple self-care treatments.
If you are experiencing certain symptoms like lack of bowel control, weakness, fever, or weight loss, or your low back pain remains after several weeks of home treatment, your doctor may wish to send you for tests. Seek medical attention immediately if you are experiencing any of these symptoms in addition to lower back pain.
Imaging tests include X-rays, computerized tomography (CT) scans, ultrasound, and magnetic resonance imaging (MRI), may be ordered so your doctor can check for bone problems, disc problems, or problems with the ligaments and tendons in your back.
If your doctor suspects a problem with the bones in your back, they may send you for a bone scan or bone density test. Electromyography (EMG) or nerve conduction tests can be ordered if a problem with your nerves is suspected.
Low Back Pain Treatment
Prevention of Low Back Pain
There are many ways in which low back pain can be prevented. Practicing prevention techniques may also help to lessen the severity of your symptoms should you experience a lower back injury. Prevention involves:
exercising the muscles in your abdomen and back
losing weight if you are overweight
lifting items properly by bending at the knees and lifting with the legs
maintaining proper posture
sleeping on a firm surface
sitting on supportive chairs that are at the correct height
avoiding high-heeled shoes
quitting smoking – nicotine degenerates spinal discs and also reduces blood flow
The spine is a column of bones. It provides stability and support for the upper body. It enables us to turn and twist. Spinal nerves run through openings in the vertebrae and conduct signals from the brain to rest of the body. These nerves are protected by the surrounding bone and tissues. If they are damaged or impaired in any way, it can affect functions such as walking, balance, and sensation.
Spinal stenosis is a condition in which the spinal column narrows and starts compressing the spinal cord. This process is typically gradual. If the narrowing is minimal, no symptoms will occur. However, too much narrowing can compress the nerves and cause problems.
Stenosis can occur anywhere along the spine. How much of the spine is affected can vary.
Spinal stenosis is also called:
pseudo-claudication
central spinal stenosis
foraminal spinal stenosis
What Are the Causes of Spinal Stenosis?
The most common cause of spinal stenosis is aging. Degenerative processes occur throughout the body as it ages. Tissues in the spine may start to thicken and bones may get bigger, compressing the nerves. Osteoarthritis and rheumatoid arthritis may also contribute to spinal stenosis. The inflammation they cause can put pressure on the cord.
Other conditions that can cause stenosis include:
spine defects present at birth
a naturally narrow spinal cord
scoliosis, or spinal curvature
Paget’s disease of the bone, which causes abnormal bone destruction and regrowth
bone tumors
achondroplasia, a type of dwarfism
Symptoms of Spinal Stenosis
Symptoms typically progress over time, as nerves become more compressed. You might experience:
leg or arm weakness
lower back pain with standing or walking
numbness in your legs or buttocks
balance problems
Sitting in a chair usually helps relieve these symptoms. However, they will return with periods of standing or walking.
How Is Spinal Stenosis Diagnosed?
If you experience symptoms of spinal stenosis, your doctor will start by taking a medical history, performing a physical exam, and observing your movements. Tests can be used to confirm a suspected diagnosis. They may include:
spinal imaging, using X-ray, MRI, or CT scan
electromyelogram (EMG), to check the health of spinal nerves
bone scan to look for damage or growths in the spine
Spondylolisthesis and Spondylolisthesis
Spondylolisthesis is a spinal condition that affects the lower vertebrae (spinal bones). This disease causes one of the lower vertebra to slip forward onto the bone directly beneath it. This is a painful condition, but it is treatable in most cases. Both therapeutic and surgical methods may be used. Proper exercise techniques can help keep this condition from developing.
Symptoms of Spondylolisthesis
The symptoms of spondylolisthesis vary. Patients with mild cases may not have any symptoms. However, people with severe cases may be unable to perform daily activities. Some of the most common symptoms are:
- persistent lower back pain
- stiffness in the back and legs
- lower back tenderness
- thigh pain
- tight hamstring and buttock muscles
Causes of Spondylolisthesis
Causes of spondylolisthesis vary based on age, heredity, and lifestyle. Children may suffer from this condition as the result of a birth defect or injury. However, patients of all ages are susceptible if the condition runs in their families. Rapid growth during adolescence may also be a contributing factor.
Playing sports may also cause overstretching of the spine and stress on the lower back. The following sports are especially likely to cause this condition:
- football
- gymnastics
- track and field
- weightlifting
Spondylolysis is often a precursor to spondylolisthesis. Spondylolysis occurs when there is a fracture in a vertebra, but it has not yet fallen onto a lower bone in the spine.
Diagnosing Spondylolisthesis
Physical exams are the first step in diagnosing this condition. Patients with spondylolisthesis may have difficulty raising a leg straight outward during simple exercises. X-rays of the lower spine are crucial for determining whether a vertebra is out of place. Your doctor may also look for any possible bone fractures on the X-ray images.
Your doctor may order a more detailed computerized tomography (CT) scan if the misplaced bone is pressing on your nerves.
Treating Spondylolisthesis
The treatment for spondylolisthesis depends on the severity of pain and vertebra slippage. Nonsurgical treatments can help ease pain and encourage the bone to go back into place. It’s important to avoid contact sports during the healing process.
Common nonsurgical treatment methods include:
- wearing a back brace
- physical therapy exercises
- taking over-the-counter or prescription anti-inflammatory drugs (such as ibuprofen) to reduce pain
- epidural steroid injections
Potential Complications
Medical intervention is crucial for relieving symptoms of spondylolisthesis. This condition can cause chronic pain and permanent damage if left untreated. Patients may eventually experience joint weakness and leg paralysis if nerve damage is present. Infection of the spine may also occur in rare cases.
Sciatica
Your sciatic nerve begins at your spinal cord, goes through your hips and buttocks, and then branches down each leg. This nerve is the body’s longest nerve and one of the most important ones, as it has a direct effect on your ability to control and feel your legs. When this nerve is irritated, you will experience sciatica.
Sciatica is a sensation that can manifest itself as a moderate to excruciating pain that you feel in your back, buttocks, and legs. You may also feel weakness or numbness in these areas. Sciatica is a symptom caused by an underlying injury to the nerve or to an area that impacts the nerve, such as your vertebrae (the bones in the neck and back).
What Causes Sciatica?
Sciatica can be caused by a number of conditions that involve the spine and that can affect the nerves running along your back. Other times, the cause is an injury, such as falling or spinal/sciatic nerve tumors.
Common conditions that can cause sciatica are described below.
Herniated Disks
Your vertebrae, or spinal bones, are separated by pieces of cartilage. Cartilage is filled with a thick, clear material to ensure flexibility and cushioning while you move around. Herniated disks occur when the first layer of the cartilage rips. The substance inside can extrude and compress the sciatic nerve, resulting in lower limb pain and numbness. It is estimated that one in every 50 people will experience a herniated disk in their lifetime, according
Spinal Stenosis
Also called lumbar spinal stenosis, this condition is characterized by the abnormal narrowing of the upper or lower spinal canal. This narrowing puts pressure on the spinal cord and the sciatic nerve roots.
Spondylolisthesis
This is one of the associated conditions of degenerative disk disorder. When one spinal bone (vertebra) extends forward over another, the extended spinal bone can pinch your sciatic nerve.
Piriformis Syndrome
Piriformis syndrome is a rare neuromuscular disorder in which the piriformis muscle (the muscle that connects the lower portion of your spine to your thighbones) involuntarily contracts or tightens, causing sciatica. The sciatica occurs because of the pressure the tightening places on the sciatic nerve. Piriformis syndrome can worsen as the result of such commonplace events as sitting for long periods of time, falling, or being involved in a fender-bender.
Symptoms of Sciatica
Sciatica is a very distinct type of symptom. If you are experiencing pain that flows from your lower back through your buttock area and into your lower limbs, it is typically sciatica.
Sciatica is the result of damage or injury to the sciatic nerve, so other symptoms of nerve damage are usually present with the pain. Other symptoms of sciatica may include:
pain that gets worse with movement
numbness/weakness: This symptom can occur in your legs or feet and is usually felt along the sciatic nerve pathway. In severe cases, there can be a loss of feeling and/or movement.
pins and needles: This is a painful tingling in your toes or feet.
incontinence: This is the term for the inability to control your bladder or bowels. This is a rare symptom of cauda equina syndrome (which is explained ahead) and calls for immediate emergency attention.
When to Seek Medical Attention
Seek immediate medical attention in the case of the following symptoms:
Your pain comes after a severe injury or accident.
You have sudden, excruciating pain in your lower back or leg that is coupled with numbness or muscle weakness in that same leg.
You are not able to control your bladder or bowels (symptom of cauda equina syndrome).
Cauda Equina Syndrome
This is a rare disorder that can cause paralysis, chronic bladder and bowel issues, and decreased sexual sensation if left untreated. Because this disorder often develops slowly, when symptoms appear, it is important to make an appointment with your doctor immediately.
Symptoms of this disorder include:
inability to control your bladder or bowels (this includes retaining waste as well)
pain, numbness, or weakness in one or both of your legs, making it hard to get up after sitting; you may notice yourself stumbling when trying to get up
a noticeable progression or sudden severe loss of feeling in your lower body area, which includes the area between the legs, the buttocks, the inner thighs, the backs of the legs, and the heels and entire foot
Diagnosing Sciatica
Since sciatica is, itself, a symptom that can vary from condition to condition and person to person, your doctor will first want to get your full medical background. This includes whether or not you have had any recent injuries, where you feel the pain, and how the pain feels. The next step is a physical exam that will include testing your muscle strength and reflexes. Your doctor might also have you do some stretching and moving exercises to determine which ones bring about more pain.
Treatment of Sciatica
Upon first diagnosis of sciatica, your doctor will often give you tips for treating your sciatica pain. One of the most important things to remember is to keep your daily activities going as much as possible, as lying in bed or avoiding activity can create a worse situation than you started with.
At-Home Treatments
Some commonly suggested at-home treatments are described below.
Cold Remedy
You can purchase ice packs or even use a package of frozen vegetables. Wrap the ice pack or frozen vegetables in a towel and then apply to the affected area for 20 minutes a day, several times a day during the first few days of pain. This will help to reduce swelling and ease pain.
Hot Remedy
You can also purchase hot packs or a heating pad. It is recommended that you use ice the first couple of days. After two or three days, switch to heat. If you continue to have pain, try alternating between ice and heat therapy.
Stretching
Gentle stretching of the lower back can also be helpful. A good way to do quality stretching is to get personal, one-on-one physical therapy or even yoga instruction from a physical therapist or instructor who is aware of and trained in dealing with your injury.
Over-the-Counter Medication
Over-the-counter medications, such as aspirin and ibuprofen, can also help with pain, inflammation and swelling. Be careful using aspirin excessively due to its potential complications, which include stomach bleeding and ulcers.
Regular Exercise
The more you stay active, the more endorphins your body releases. Endorphins are painkillers made by the body. Keep to low-impact activities at first, such as swimming and stationary bicycling. As your pain decreases and your endurance improves, create an exercise regimen that includes aerobics, core stability, and strength training. A regimen with these components can decrease the risk of future back problems.
physical therapy: Exercises will help to improve posture and strengthen back muscles.
.
Risk Factors for Developing Sciatica
Certain behaviors or factors can make sciatica more likely. The most common factors for developing sciatica include:
age: As your body ages, it becomes more likely that parts will wear out or break down.
occupation: Certain careers place a lot of strain on your back, especially those that involve lifting heavy objects, sitting for extended periods, or twisting movement.
diabetes: This condition can increase the risk of nerve damage.
smoking: Smoking can cause the outer layer of your spinal disks to break down.
Alternative Treatments for Sciatica
How to Prevent Sciatica
The following steps can assist you in preventing sciatica or from keeping it from reoccurring:
Exercise often. Strengthening your back muscles and your stomach or core muscles is the key to maintaining a healthy back.
Mind your posture. Make sure your chairs offer proper support for your back. You should be able to place your feet on the floor, and make sure to use your armrests.
Mind how you move. Take care of yourself. Lift heavy objects the proper way by bending at the knees and keeping your back straight.
Scoliosis is an abnormal curvature of the spine. The human spine is made of bones called vertebrae that are stacked on top of one another. This flexible structure allows us to bend and twist our bodies in all directions.
A healthy spine curves from front to back at the neck, chest and lower back. However, in people with scoliosis, the spine also develops a side-to-side curvature. This usually happens during the growth spurt that begins just before puberty.
A scoliosis curve can be C- or S-shaped. In severe cases, the spine will rotate and twist, causing the ribs to stick out more on one side.
Most cases of scoliosis are mild and cause no health problems. In severe cases, the twisting of the spine and ribs reduces space within the chest cavity. This can interfere with breathing and put strain on the heart. Untreated scoliosis can also compress and damage the spinal nerves, leading to paralysis. However, these complications are very rare in the United States, because most cases are treated in their early stages.
Scoliosis affects about 3 in every 100 people, or about 6 million people in the United States. It can appear at any age, but usually starts between ages 9 and 15. While scoliosis is equally common in boys and girls, girls are eight times more likely to have severe curves that require treatment.
Causes
In 80–۸۵ percent of scoliosis cases, the cause is unknown. This type of scoliosis is called “idiopathic,” meaning “of unknown origin.” Genetics may play a role in cases of idiopathic scoliosis; about 30 percent of children with this type of scoliosis have a close relative with the condition.
In a few cases, scoliosis is caused by another underlying medical condition such as cerebral palsy, muscular dystrophy, injury or infection. These conditions can cause muscle weakness and imbalance, which in turn can cause the spine to curve as it grows.
Scoliosis can also result if the bones of the spine do not form properly or separate before birth. Cases of this kind are called “congenital scoliosis.”
Symptoms
Mild scoliosis can be difficult to detect, because it usually doesn’t cause pain or discomfort. Early symptoms include:
- Uneven shoulders
- Uneven waist
- One shoulder blade sticks out more than the other
- One hip is higher than the other.
In more severe cases, you might notice:
- Ribs stick out further on one side than the other
- Back pain
- Difficulty breathing.
See your doctor if you or your child have symptoms of scoliosis. Early detection and treatment can help to prevent the curve from worsening.
Diagnosis
About half of all schools routinely screen students for scoliosis. The test involves bending over and touching your toes so that a doctor or nurse can examine the position of your spine and ribs.
Diagnosis for scoliosis starts with a physical exam. Your doctor will have you assume different postures to check for evenness of the shoulders, hips and ribs. You also might receive a neurological exam to detect weakness, numbness or abnormal reflexes.
In most cases, a simple X-ray can confirm a diagnosis of scoliosis and show how far the curve has progressed. Children with scoliosis are usually referred to a specialist called an orthopedist or orthopedic surgeon for treatment.
Lordosis, also known as swayback, is a condition in which the spine in the lower back has an excessive curvature. The spine naturally curves at the neck, upper back, and lower back to help absorb shock and support the weight of the head. Lordosis occurs when the natural arch in the lower back, or lumbar region, curves more than normal. This can lead to excess pressure on the spine, causing pain.
People with lordosis often have a visible arch in their lower backs. When looking at them from the side, their lower backs form a defined “C” shape. In addition, people with swayback appear to be sticking out their stomachs and buttocks.
The easiest way to check for lordosis is to lie on your back on a hard surface. You should be able to slide your hand under your lower back, with little space to spare. If you have lordosis, you will have extra space between your hand and your low back.
Common Causes of Lordosis
Often, lordosis appears in childhood without any known cause. This is called benign juvenile lordosis. However, lordosis can affect people of any age.
Other potential causes of lordosis include:
- poor posture
- obesity
- osteoporosis (weakening of the bones with age)
- discitis (a disorder of the disks between the spinal vertebrae)
- kyphosis (an excessive outward curvature at the mid-back)
- spondylolisthesis (a condition in which one vertebra slips forward or backward relative to the next vertabra)
- achondroplasia (a form of dwarfism)
When to Seek Treatment for Lordosis
If the lordotic curve corrects itself when you bend forward (i.e. the curve is flexible), you do not need to seek treatment. However, if you bend over and the lordotic curve remains (i.e. the curve is not flexible), you should seek treatment.
In addition, you should seek treatment if you experience any of the following:
- pain
- muscle spasms
- tingling or numbness
- bladder or bowel difficulties
Much of our flexibility, mobility, and activity depend on the health of the spine. Getting treatment to help correct the curvature can help prevent complications later in life, such as arthritis and chronic back pain
The upper back (thoracic spine) comprises of many bones known as vertebrae. There are 12 thoracic vertebrae named T1 to T12 from the top of the upper back to the bottom of the upper back. Each of these vertebrae connects with the vertebra above and below via two types of joints: the facet joints on either side of the spine and the discs centrally (figure 1). These joints are designed to support body weight and enable spinal movement. In close proximity to these joints are nerves, which can be damaged or irritated upon injury to either the disc or the facet joint at a particular level (figure 1).
During certain movements of the spine, stretching or compressive forces are placed on the facet joints and discs at the T4 level. If these forces are excessive and beyond what the joints can withstand, injury to the facet joints or discs may occur. When this results in irritation or damage to the adjacent nerves at the T4 level and the patient experiences diffuse arm pain, pins and needles or numbness in the upper arm the condition is known as T4 syndrome.
Causes of T4 syndrome
T4 syndrome typically occurs due to injury to the facet joints or disc at T4 which then affects the nerve root at that level. Injury to these structures can occur during excessive bending, lifting, arching, or twisting movements or due to poor posture. This may occur traumatically or due to repetitive or prolonged forces.
Signs and symptoms of T4 syndrome
Patients with this condition usually experience diffuse arm pain and sensory symptoms such as pins and needles or numbness in the upper arm. Pain may also be felt in the upper back and occasionally, the neck may be affected.
Symptoms may develop suddenly during the causative activity, however, it is also common for patients to experience pain and stiffness after the provocative activity, particularly the next morning. Symptoms are typically felt in one arm or on one side of the upper back although occasionally both sides may be affected. Pain may also be referred into the shoulder blade, ribs and chest. Muscle spasm, stiffness and restricted spinal movement may also be experienced, particularly around the affected joint. Symptoms are generally exacerbated with activities that involve twisting, lifting, arching backwards, bending forwards or sideways, sitting for prolonged periods of time, coughing or sneezing, or performing activities that involve using the hands in front of the body such as driving or ironing.
Diagnosis of T4 syndrome
A thorough subjective and objective examination from a physiotherapist is usually sufficient to diagnose T4 syndrome. Investigations such as an MRI or CT scan may be required to confirm diagnosis.
What is a thoracic disc bulge?
The thoracic spine (i.e. the mid and upper back) comprises of many bones known as vertebrae, each of which is separated by a disc (figure 1). The disc comprises of many layers of strong connective tissue wrapping around the disc. In the middle of the disc lies a soft jelly-like substance which is capable of changing shape. When this jelly-like substance protrudes from the disc due to a tear in several layers of the connective tissue, this is known as a thoracic disc bulge
To understand the mechanism of a thoracic disc bulge, it is useful to liken the disc to a vanilla slice. Imagine a vanilla slice wrapped in five layers of sandwich wrap. The top and bottom layers of pastry represent the vertebra (bones), the custard represents the jelly-like substance of the disc and the sandwich wrap represents the connective tissue around the disc. If you were now to pinch the front of that vanilla slice, you could imagine, the custard would squeeze towards the back of the vanilla slice and may tear two or three layers of sandwich wrap at the back of the vanilla slice. As a result the custard is no longer supported as effectively at the back of the vanilla slice and therefore bulges out at this location. In the disc, the situation is the same. Bending forward closes down the front of the disc, pushing the jelly-like substance within the disc towards the back. Overtime or suddenly, this may tear several layers of connective tissue at the back of the disc resulting in a disc bulge.
Causes of a thoracic disc bulge
There are several activities in everyday life which typically cause thoracic disc bulges provided they are forceful, repetitive or prolonged enough. These include: bending forward, slouching, activities using your arms in front of the body (e.g. washing dishes, driving etc.) and lifting (especially in combination with twisting).
Occasionally, thoracic disc bulges may occur following a trivial movement involving bending forward such as picking up a small object or sneezing. In these instances, the disc has normally been subject to repetitive or prolonged bending, slouching or lifting forces leading up to the incident.
Signs and symptoms of a thoracic disc bulge
Patients with a thoracic disc bulge may experience a sudden onset of back pain during the causative activity, however, it is also common for patients to experience pain and stiffness after the provocative activity, particularly the next morning.
Symptoms are typically felt in the mid back, sometimes between or around the shoulder blades and may be located centrally, on one side or on both sides of the spine. The patient may experience pain radiating around the ribs and into the chest, or sometimes down the arms. Muscle spasm, pins and needles, numbness or weakness may also be present.
In some cases, patients may appear to stand with their spine noticeably out of alignment as a result of the disc bulge. Symptoms are generally exacerbated with activities involving rotation, side bending, activities using your arms in front of your body, lifting, bending forwards, or prolonged sitting (especially if slouched). Breathing, coughing, and sneezing may also aggravate symptoms.
Patients with a thoracic disc bulge often experience pain that is worse first thing in the morning.
Diagnosis of a thoracic disc bulge
A thorough subjective and objective examination from a physiotherapist is usually sufficient to diagnose a thoracic disc bulge. Investigations such as an MRI or CT scan may be required to confirm diagnosis
lumbar degenerative Disc Disease
The intervertebral discs in the lower spine are commonly blamed for low back pain. Yet low back pain has many possible causes, and doctors aren’t always certain why symptoms occur.
During an office visit for low back pain, your doctor may describe how changes in the discs can lead to back pain. When talking about these changes, your doctor may use the terms degeneration or degenerative disc disease. Although the parts of the spine do change with time and in some sense degenerate, this does not mean the spine is deteriorating and that you are headed for future pain and problems. These terms are simply a starting point for describing what occurs in the spine over time, and how the changes may explain the symptoms people feel.
Anatomy
What parts of the spine are involved?
The human spine is made up of 24 spinal bones, called vertebrae. Vertebrae are stacked on top of one another to form the spinal column. The spinal column gives the body its form. It is the body’s main upright support. The section of the spine in the lower back is known as the lumbar spine.
An intervertebral disc sits between each pair of vertebrae. The intervertebral disc is made of connective tissue. Connective tissue is the material that holds the living cells of the body together. Most connective tissue is made of fibers of a material called collagen. These fibers help the disc withstand tension and pressure.
The disc normally works like a shock absorber. It protects the spine against the daily pull of gravity. It also protects the spine during strenuous activities that put strong force on the spine, such as jumping, running, and lifting.
An intervertebral disc is made of two parts. The center, called the nucleus, is spongy. It provides most of the disc’s ability to absorb shock. The nucleus is held in place by the annulus, a series of strong ligament rings surrounding it. Ligaments are connective tissues that attach bones to other bones.
Between the vertebrae of each spinal segment are two facet joints. The facet joints are located on the back of the spinal column. There are two facet joints between each pair of vertebrae, one on each side of the spine. A facet joint is made of small, bony knobs that line up along the back of the spine. Where these knobs meet, they form a joint that connects the two vertebrae. The alignment of the facet joints of the lumbar spine allows freedom of movement as you bend forward and back.
Causes
Why do I have this problem?
Our intervertebral discs change with age, much like our hair turns gray. Conditions such as a major back injury or fracture can affect how the spine works, making the changes happen even faster. Daily wear and tear and certain types of vibration can also speed up degeneration in the spine. In addition, strong evidence suggests that smoking speeds up degeneration of the spine. Scientists have also found links among family members, showing that genetics play a role in how fast these changes occur.
Disc degeneration follows a predictable pattern. First, the nucleus in the center of the disc begins to lose its ability to absorb water. The disc becomes dehydrated. Then the nucleus becomes thick and fibrous, so that it looks much the same as the annulus. As a result, the nucleus isn’t able to absorb shock as well. Routine stress and strain begin to take a toll on the structures of the spine. Tears form around the annulus. The disc weakens. It starts to collapse, and the bones of the spine compress.
This degeneration does not always mean the disc becomes a source of pain. In fact, X-rays and MRI scans show that people with severe disc degeneration don’t always feel pain.
Symptoms
What does the condition feel like?
Pain in the center of the low back is often the first symptom patients feel. It usually starts to affect patients in their twenties and thirties. Pain tends to worsen after heavy physical activity or staying in one posture for a long time. The back may also begin to feel stiff. Resting the back eases pain. At first, symptoms only last a few days.
This type of back pain often comes and goes over the years. Doctors call this recurring back pain. Each time it strikes, the pain may seem worse than the time before. Eventually the pain may spread into the buttocks or thighs, and it may take longer for the pain to subside.
Diagnosis
How do doctors diagnose the problem?
Diagnosis begins with a complete history and physical exam. Your doctor will ask questions about your symptoms and how your problem is affecting your daily activities. Your doctor will also want to know what positions or activities make your symptoms worse or better.
Then the doctor does a physical examination by checking your posture and the amount of movement in your low back. Your doctor checks to see which back movements cause pain or other symptoms. Your skin sensation, muscle strength, and reflexes are also tested.
Doctors rely on the history and physical exam to determine which treatments will help the most. X-rays are rarely ordered on the first doctor visit for this problem. This is because over 30 percent of low back X-rays show abnormalities from degeneration, even in people who aren’t having symptoms.
However, if symptoms are severe and aren’t going away, the doctor may order an X-ray. The test can show if one or more discs has started to collapse. It can also show if there are bone spurs in the vertebrae and facet joints. Bone spurs are small points of bone that form with degeneration.
When more information is needed, your doctor may order a magnetic resonance imaging (MRI) scan. The MRI machine uses magnetic waves rather than X-rays to show the soft tissues of the body. It is helpful for showing if the tissues in the disc are able to absorb water and whether there are cracks inside the disc. It can also show if there are problems in other soft tissues, such as the spinal nerves.
Discography can help with the diagnosis. This is a specialized X-ray test in which dye is injected into one or more discs. The dye is seen on X-ray and can give some information about the health of the disc or discs. This test may be done when the surgeon is considering surgery, since it can help determine which disc is causing the symptoms.
What is postural syndrome?
Postural syndrome of the upper back is a relatively common condition that causes pain in the upper back without significant damage or trauma to tissue. Patients with this condition only experience an ache or pain during activities placing sustained stress on normal tissue.
The mechanism of pain onset in postural syndrome can be demonstrated by gently bending your index finger backwards until you feel a stretch (figure 1).
At this point there is no tissue damage or pain, however, if you maintain this position for long enough, your finger will gradually become painful or ache. Once the finger is released and allowed to change position, the pain or ache will ease. Postural syndrome in the upper back occurs in a similar fashion and typically occurs due to sitting or standing in poor positions for prolonged periods of time (figures 2, 3 and 4).
When standing or sitting slouched (figures 2 and 3), the bend in your upper back and arch in your upper neck increases (figure 4). In addition your shoulders typically move forwards. This places considerable stretching force and increased load on the joints and muscles of your upper back and neck and will gradually cause an ache or pain if sustained for too long. When this occurs the condition is known as postural syndrome.
Causes of postural syndrome
Postural syndrome is a condition that is caused by adopting poor posture over a prolonged period of time. This may occur in any position such as standing or lying, but is particularly common during sitting (e.g. at a computer, using a mobile phone, watching television or driving).
Postural syndrome is also relatively common during everyday activities that encourage the arms to move forward in front of the body such as cooking, cleaning, gardening or ironing.
In sport, postural syndrome is often seen in athletes whose activity involves prolonged bending forward postures such as cycling, hockey players, baseball catchers and wicket keepers in cricket.
Signs and symptoms of postural syndrome
Patients with postural syndrome typically have normal, pain-free movement. Symptoms are only experienced when poor posture is maintained for prolonged periods. This can occur in any position (e.g. sitting, standing, lying etc.).
Pain is typically experienced as a dull ache or burning sensation in the upper back and can sometimes be accompanied by symptoms in the neck, lower back or shoulders. Usually the pain associated with postural syndrome will quickly ease upon moving or changing positions, thereby taking the strain off the affected structures.
Diagnosis of postural syndrome
A thorough subjective and objective examination from a physiotherapist is usually sufficient to diagnose postural syndrome of the upper back. Investigations such as an X-ray, MRI or CT scan may be required, in rare cases, to rule out other
Diseases
-
Neck Pain
-
Shoulder & Elbow
-
Hand & Wrist
-
Arthritis
-
Lower Back Pain
-
Hip & Femur
-
Knee & Lower Leg
-
Foot & Ankle
-
Osteoporosis