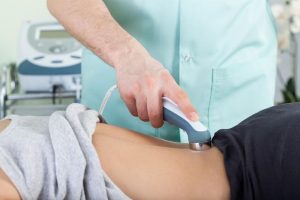
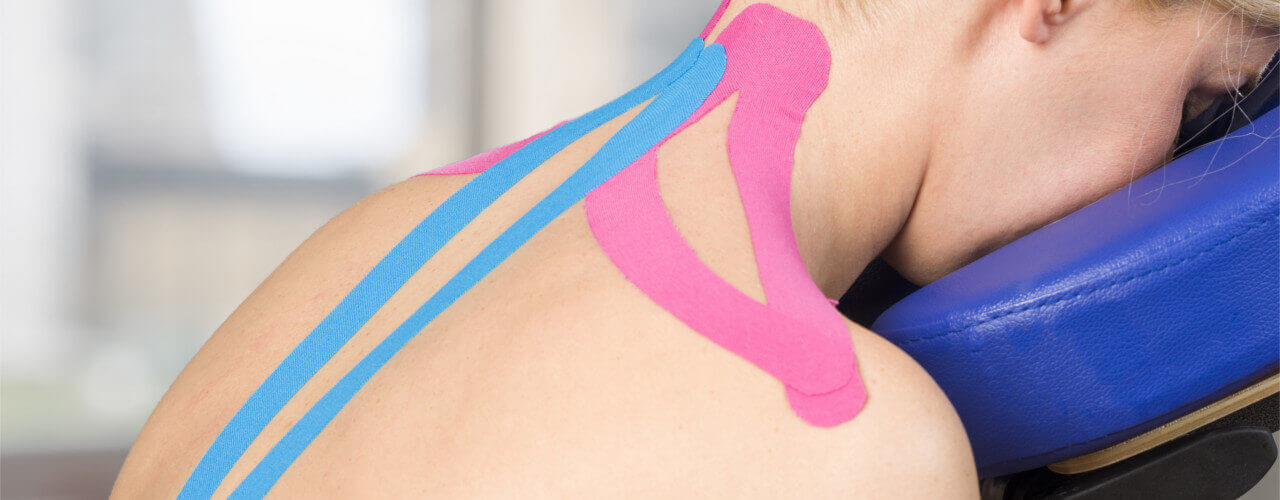
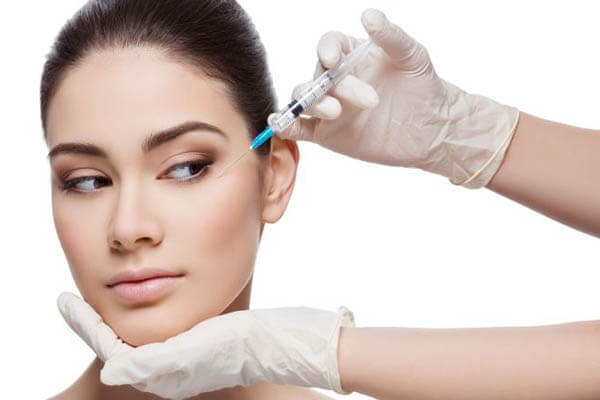
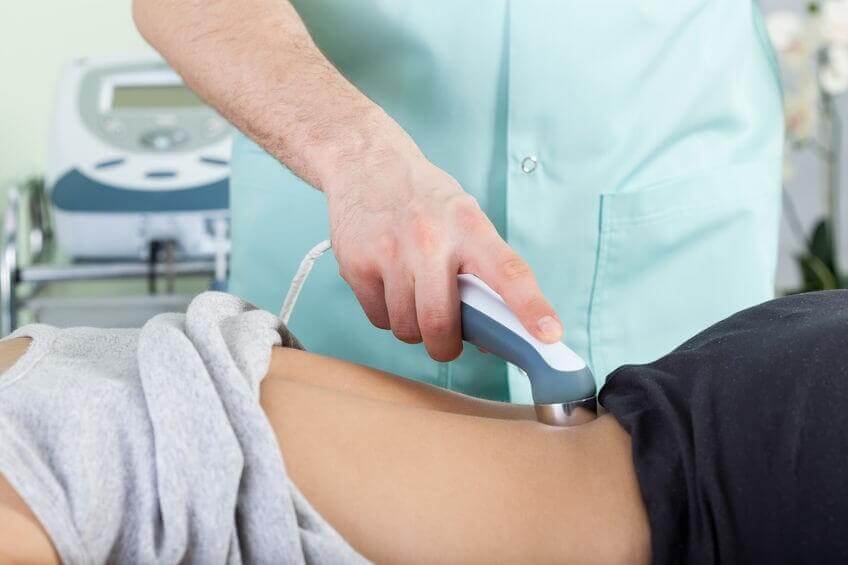
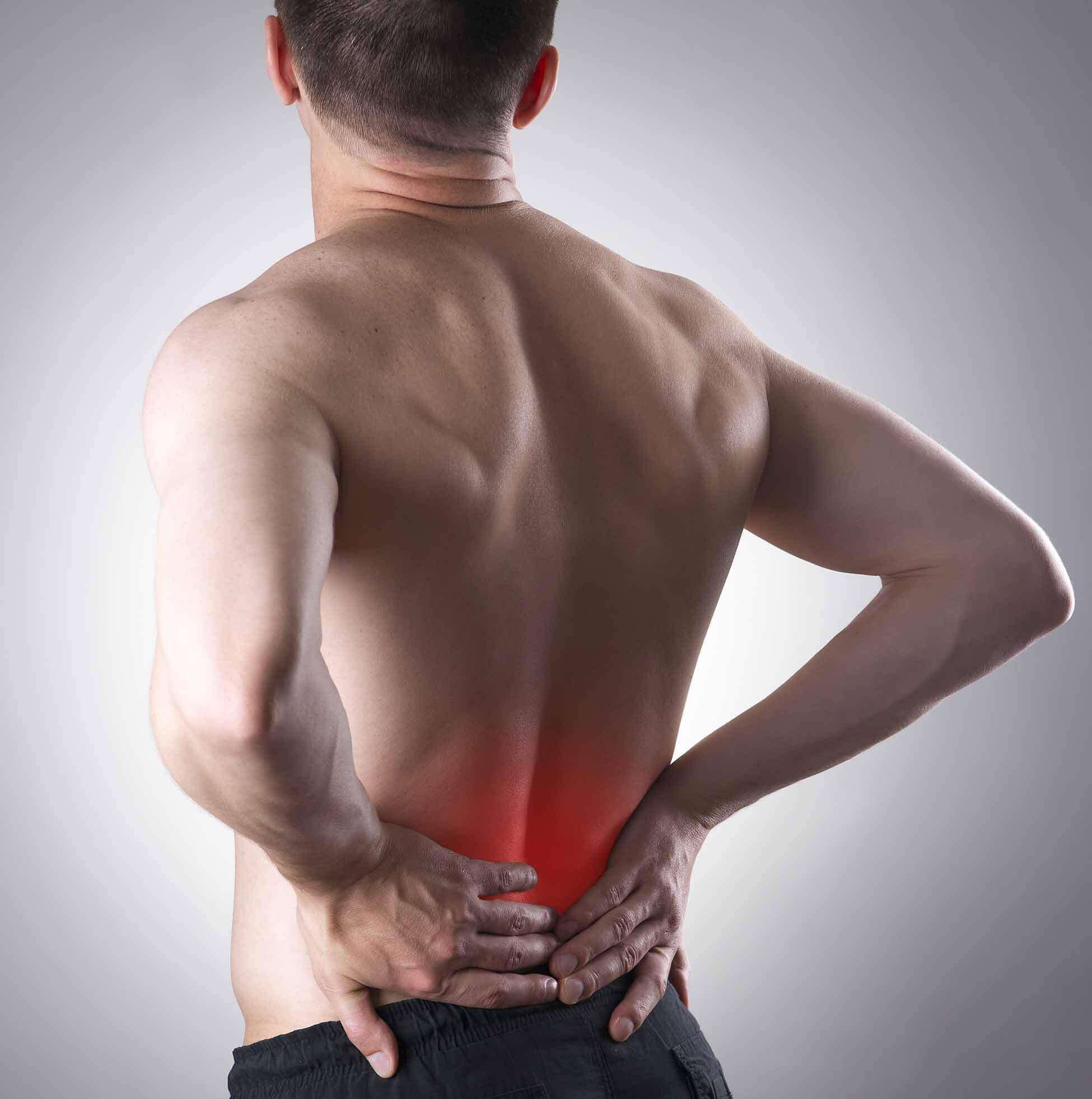
Intra-canal injections of the spinal cord under fluoroscopy

Fluoroscopic injections for the treatment of back problems
Specific fluoroscopic injections to treat neck and lumbar disorders are one of the key components of a rehabilitation program, with specialists utilizing it along with physiotherapy, exercise therapy and drug administration to achieve optimal results. Therefore, the patient must carefully follow the physician’s instructions for the treatment to be successful.
How is the need and type of injections diagnosed under fluoroscopy?
Dr. alireza moghtaderi, a pain relief specialist, determines the suitability of these injections after a thorough and thorough examination based on the results of tests and the results of tests such as ultrasound, muscle strips and MRI images, CT scans and bone scans, and patient symptoms. Dr. alireza moghtaderi then suggests the appropriate type of injection.
Classification of injections under fluoroscopy
Various fluoroscopic injections are performed in Dr. alireza moghtaderi office, each targeting specific spine structures. All closed surgeries can be divided into two main groups:
Diagnostic block: Diagnostic block is performed when the origin of the pain is not specified. By doing this, Dr. alireza moghtaderi will determine which spine structure causes the symptoms.
Treatment Blocks: The steroid injected in this closed surgery does not strengthen the muscles and is quite different from the drug used in bodybuilding and bodybuilding. The steroid is injected to reduce inflammation and consequently relieve pain.
Treatable problems with closed spine surgery
Not all patients can be closed surgery and some complications cannot be treated with non-surgical methods. Some neck and back problems that can be treated with closed surgery include:
Arthritis of the Waist and Neck
Cervical Disc
Waist disc
back ache
Sciatica
Spinal fracture (spondylolisthesis)
Types of injections under fluoroscopy
Fast block joint
The fast articular block is both a test and a treatment. The medicine injected into the fastener should anesthetize this joint. If the pain is relieved after the injection, the doctor can determine the origin of the pain. Cortisone is sometimes injected with anesthesia to reduce inflammation in the joint and relieve pain for several weeks or months. Of course, pain relief is usually temporary.
Action
The doctor inserts a long needle into the fastener center (s). The needle enters the body from behind. The anesthetic is injected into the waist skin at the needle insertion site to relieve the patient with this local anesthesia. The doctor uses a fluoroscope when inserting the needle to make sure the needle is inserted into the fastener joint. A fluoroscope is a special X-ray display that allows the physician to see the spine and the needle as it moves. The doctor, after making sure the needle is in the fastener, injects the combination of anesthetic (for example, novacaine) and cortisone into the joint.
Complications
Arthritis infection and allergic reaction to injectable drugs are one of the possible complications of fasting joint.
Ozone Therapy
There are many different ways to deliver oxygen to cells using either hydrogen peroxide or ozone. The ozone therapy described in this article should only be performed by a specialist.
Action
Ozone Infusion Pump Therapy: Some blood is taken from the patient and pumped into the infusion pump, then the ozone gas is pumped into the pump and mixed with gentle shaking of the blood. After this, the pale red blood is re-injected into the patient’s body. Ozone therapy is usually performed twice a week or month, depending on the severity of the complication, and relieves the pain for several weeks or months.
Complications
Ozone therapy is completely safe and has no side effects. In fact, it has been proven that ozone therapy is the safest treatment ever devised.
Plasma Rich Plasma Therapy (PRP)
Plasma rich in platelets, or PRPs, is human blood, which is dissolved after rotation to obtain a high concentration of platelets. Platelets are blood coagulant cells that also accelerate the process of muscle, tendon and ligament healing. According to research, platelets release growth factors that give new force to the healing cells, thus improving tissue repair and accelerating soft tissue healing.
Action
The injection of PRP does not take more than an hour and during this time the PRP solution is prepared according to the procedure described above. The plasma-rich portion is separated and injected into a disc, muscle or damaged joint that has been diagnosed as a source of pain and does not heal well. Your doctor will help with radiography (eg fluoroscopy) at the time of injection into the spine structures to ensure that the PRP injection is performed safely and appropriately in the affected area. The upper body ultrasound is also usually used for PRP injection in the painful area.
Complications
PRP is generally a very safe treatment that does not cause any allergies because the patient’s own blood is used. However, with any operation that the needle enters the body, there is a risk of infection, bleeding and nerve damage. Of course, these complications rarely occur. Other complications depend on the area being treated.
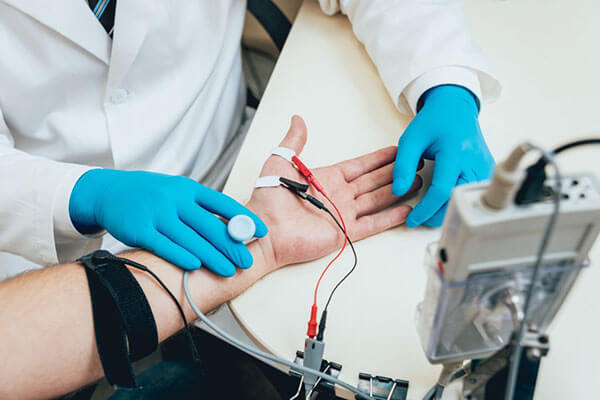
Radiofrequency
Radiofrequency waves are electromagnetic waves that travel at the speed of light. Radio frequency energy is a type of heat energy produced by a special generator at very high frequencies. The heat energy is generated using this generator and is carefully transmitted to the nerves carrying the pain message. “Injury” involves the spherical area of tissue destruction at the tip of the RF needle, which also includes the nerves that carry the pain message.
Action
With fluoroscopic guidance (live video radiography) a small insulated needle or RF canal is placed next to the pain transmitting nerve. The cannula piston is covered with protective insulation except for the last 2 to 5 mm to allow only electrical current to flow through the peripheral tissues. The physician releases a small amount of electricity through the needle tip at two different frequencies after making sure the cannula is in place for testing. Successful testing confirms the correct location of the cannula. The next step is to inject the anesthetic into the treated area. The cannula tip is then heated with the RF generator for 5 seconds and the target nerve is destroyed.
Complications
Patients often receive mild intravenous sedation during the procedure, but this is not necessary. Strong sedative is not a substitute for safety and is not used in radio frequency practice. Neck pain or back pain usually worsens after radiofrequency for several days and then improves.
Injection into the epidural space
In closed surgery, steroid injections into the epidural space are injected with long-term anti-inflammatory drug in the epidural space. The area of the spinal cord and the spinal cord nerves are called the epidural space. The injected drug reduces swelling around the disc and nerve; swelling in turn is associated with reduced pain, nausea and anesthesia or other symptoms caused by nerve irritation / inflammation or loss of tissue swelling.
Action
The injection itself takes only a few minutes. To do this, the needle enters the skin because, with minor discomfort, the elusive doctor anesthetizes the skin and deeper tissues with a topical anesthetic that is injected with a very fine needle. The lumbar skin is cleansed with a disinfectant before steroid injection.
Complications
The patient feels a slight pressure at the injection site after the injection. This pressure is due to the drug entering the body and relieves after a few hours. The back may be painful for up to a day or two due to the mechanical needle insertion process.